Best Food for Dogs With Allergies — The Vet-Backed Diet That Stops Itching Faster
Best Food for Dogs With Allergies—start with a vet-recommended hydrolyzed or novel protein diet to stop the itch. Follow an 8 to 12 week elimination plan with shopping tips for Europe and safe prescription alternatives so you can reduce scratching, ear infections, and digestive upset fast. Learn step-by-step feeding rules, Best Food for Dogs With Allergies, common mistakes to avoid, and a controlled rechallenge to confirm triggers for clear vet-backed relief today.
If your dog is rough rubbing, or getting repeated ear infections, this pillar piece gives an evidence-aware plan for diagnosing and managing Food Allergy using fast. You’ll get a vet-aware 8–12 week elimination code, clear outcome steps for choosing hydrolyzed vs novel vs limited-ingredient vs home-cooked approaches, Best Food for Dogs With Allergies a Europe-determined shopping checklist, a comparison of common owner mistakes, freedom notes for puppies and brachycephalic breeds, and a printable action BILL you can publish or hand to the audience.
How to Identify Food Allergies in Dogs — Is Your Dog’s Food the Real Problem?
Intended outcome: classify likely JOCKEY(food vs environment) so you can pick an APT diagnostic path.
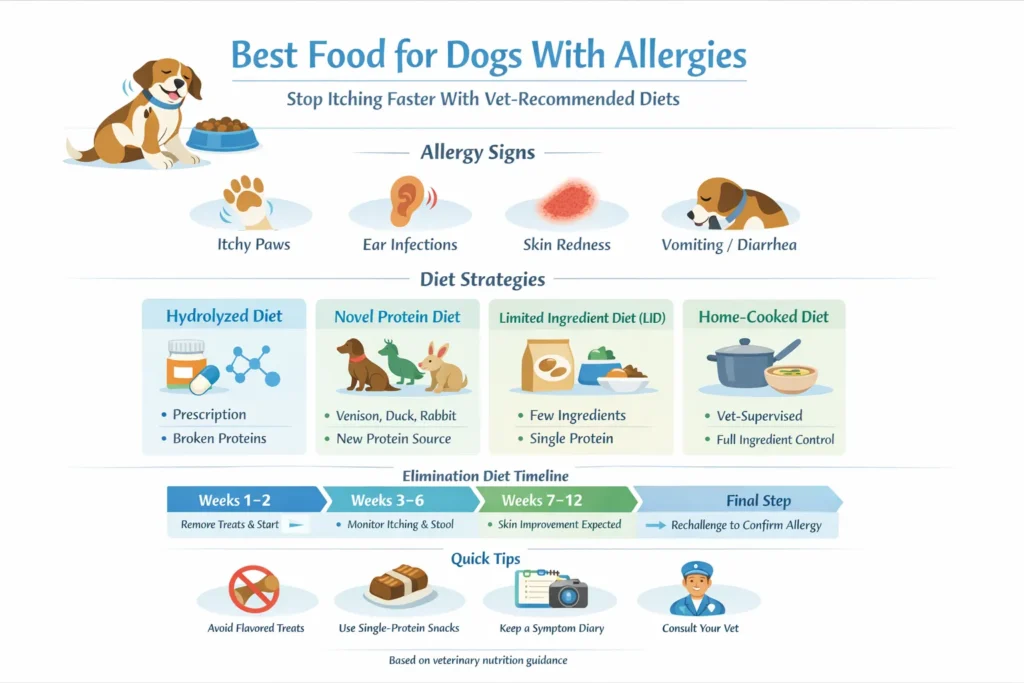
Food-allergy signals (pattern-match):
- Year-round pruritus focused on the face, paws, and ears.
- Recurrent otitis externa (smelly, waxy ears).
- Gastrointestinal signs (chronic or intermittent vomiting, loose stool) are coincident with skin signs.
- Outset or marked worsening after a diet change or introduction of new treats.
- No seasonal pattern; signs go on during low pollen months.
Environmental-allergy signals (pattern-match):
- repetitive or weather-related flares (e.g., spring pollen spike).
- deep rubbing or head-shaking after being outside in specific locations.
- Clear earthly relationship to walks/parks/grooming or risk to other animals.
- Itch rich around contact surfaces (belly, chest) or urgent urticaria/hives after outdoor exposure.
Quick action heuristic: often photos and a short syndrome vector (itch score 0–10, stool kid ear odor) for 2–4 weeks. If symptoms are steady and non-seasonal, bias toward food-elimination diagnostics. Note: the diagnostic gold standard for food allergy is a severe elimination diet followed by a controlled rechallenge — in-clinic blood IgE trial, or many skin tests do not reliably confirm food allergy only.
The four diet strategies explained — what they are & when to route to each
We present four core diet strategies as discrete diagnostic/therapeutic nodes. Use the decision tree below when choosing an initial path.
Strategy A — Hydrolyzed protein diets (prescription) — route when: moderate-to-severe disease, prior multiple protein exposures, or prior failed OTC trials
What it is: Proteins are enzymatically reduced into small peptides, decreasing immunoreactivity.
When to use: proved or complex cases; when owner compliance with strict OTC LID is doubtful; when cross-reactivity is imagined.
Pros: High clinical service in diagnostic and management contexts; formulated as nutritionally complete.
Cons: Prescription-only in many markets, higher cost, and some dogs remain reactive in unlikely facts
Strategy B — Novel-protein diets (OTC) — route when: suspected single-protein sensitivity with clean exposure history
What it is: Commercial food using proteins rarely fed to that dog historically (e.g., venison, rabbit, duck, ant).
When to use: First at-home bid for mild suspected food allergies when the owner can guarantee no prior risk.
Pros: Good palatability, accessible in many European markets, lower immediate cost than the drug
Cons: Contamination risk and mislabeled products in low-cost lines.
Strategy C — Limited-ingredient diets (LID) — route when: stepwise isolation testing or mild symptoms
What it is: junk with a reduced list of belly (often single protein + single carbohydrate).
When to use: Troubleshooting and identifying the offending ingredient in a controlled, stepwise manner.
Pros: Cheap, easy to manage for owners; useful for incremental testing.
Cons: “Limited” doesn’t guarantee no cross-contact; careful label checks are required.
Strategy D — Home-cooked / single-protein elimination diets — route when: all commercial options fail or complex multi-reactive cases
What it is: Cooked recipes using a single protein and carbohydrate source formulated under veterinary nutrition guidance.
When to use: When commercial diets cause reactions or the owner needs absolute ingredient control.
Pros: Maximum control; useful for complex or multi-sensitized patients.
Cons: Time-consuming; risk of nutritional imbalance unless formulated by a vet or board-certified veterinary nutritionist
Step-by-step elimination diet plan — structured protocol
High-level instruction: Strictness matters. Even a single flavored supplement or chew can invalidate results. Skin signs often need 8–12 weeks to clear; GI signs may improve in 2–4 weeks.
Phase A — Preparation
- Baseline media capture: take high-quality photos of face, paws, ears, and body. Save with date stamps.
- Symptom diary template: daily itch score (0–10), stool quality (Bristol-type note), ear odor/ discharge, meds used.
- Eliminate all extras: remove treats, chews, flavored medication, table scraps, dental chews, and flavored topical collars. Even flavored tablets or palatable pill pockets can contain proteins.
- Select trial diet using decision tree: mild suspicion → OTC novel-protein LID; severe/complex → discuss hydrolyzed diet with your vet.
- Purchase only allowed snacks: single-ingredient freeze-dried matching the trial protein, or use kibble pieces from the trial food.
B — Strict feeding
- Feed only the trial diet. No other foods, no raw, no scavenging.
- Avoid cross-contact: store trial food separately, inform household/family about strictness.
- Record daily entries and take weekly photos.
- Veterinary progress checks: schedule rechecks at week 4 and week 8; consider week 12 if progress is slow.
- Medication tapering: only under vet supervision. Do not stop anti-pruritic or ear meds unadvisedly; instead, work with your vet to taper and assess.
Phase C — Evaluate progress/criteria
- GI improvement: often seen within 2–4 weeks.
- Dermatologic improvement: Typically requires 8–12 weeks for a meaningful reduction in itch and ear episodes.
- Clear improvement definition: ≥50% reduction in itch score and fewer or no otitis episodes; improved coat and reduced erythema.
Phase D — Rechallenge
- Controlled rechallenge under vet supervision: reintroduce old diet or single suspect protein for a defined period (days to 14 days).
- Interpretation: Quick return of signs confirms the offending protein. If no return, consider sequential reintroduction of single proteins or alternative diagnostic routes.
Printable checklist suggestion for publication: a one-page PDF with Phase A–D steps, a daily symptom table, and decision prompts for owners and clinicians.
Which commercial foods to try — shopping checklist & categories
Shopping checklist (practical filters):
- Type (hydrolyzed, novel, LID) — select based on decision tree.
- Single animal protein is clearly listed on the front and in the ingredients.
- Manufacturer transparency: label statements about shared equipment or dedicated lines.
- Label indicates “complete & balanced” and notes compliance with regional standards.
- Wet food options exist for palatability; consider a wet + dry approach if needed.
- Buy from official EU distributors or clinics for prescriptions to avoid fakes.
Product categories & selection heuristics
- Prescription hydrolyzed lines: use for complex or confirmed allergy; available via veterinary clinics.
- Novel-protein OTC lines: venison, rabbit, duck, insect proteins — ensure the dog has minimal prior exposure to the chosen protein.
- Limited-ingredient brands: Use when you want a short ingredient list for stepwise testing.
- Single-ingredient treats: freeze-dried meats or vegetable crisps that match the trial protein.
Label red flags
- Ambiguous protein names like “meat meal” or “poultry” without specificity.
- No statement regarding equipment sharing.
- Multiple flavors or gravy coatings that introduce hidden proteins.
- Import warnings or unclear supplier data—buy from reputable EU vendors.
Note: grain-free approaches rarely help true food allergy (which is most often protein-driven) and can have unrelated health implications; do not default to grain-free for allergy control.
Comparison table — Hydrolyzed vs Novel vs LID vs Home-cooked
| Feature | Hydrolyzed (prescription) | Novel protein (OTC) | Limited-ingredient (OTC) | Home-cooked (vet planned) |
| Diagnostic accuracy | High | Moderate | Moderate | High (if controlled) |
| Cross-contamination risk | Low | Medium | Medium | Low (if controlled) |
| Veterinary supervision required | Yes | Optional | Optional | Yes |
| Cost | High | Medium | Low–Medium | Variable (potentially high) |
| Palatability | Variable | Usually good | Usually good | Depends on recipe |
| Nutritional completeness | Guaranteed (clinic formula) | Check label | Check label | Must be formulated by a professional |
Clinical notes: Hydrolyzed diets are commonly chosen by vets for diagnostic and management reasons because the hydrolysis process reduces antigenicity; however, in mild cases, an OTC novel protein can be an accessible first step.
Real-life example — short case flow
Sofia (Barcelona) — 4-year-old Labrador
- History: chronic otitis externa and facial rubbing for 6 months; commercial chicken kibble.
- Decision node: moderate symptoms, but owner prefers initial at-home trial → novel-protein venison LID chosen.
- Protocol: strict elimination, weekly photos, recheck at 4 and 8 weeks.
- Outcome: modest improvement at week 6; marked improvement and resolution of ear infections at week 10. Controlled rechallenge with chicken at week 11 produced itching within 48 hours → confirmed chicken allergy. Plan: lifelong venison single-protein diet with approved single-ingredient treats.
Common mistakes owners make& how to avoid them
- Giving unauthorized treats — even one flavored chew ruins a trial. Mitigation: remove/hide all non-trial foods; use trial kibble as treats.
- Switching diets too quickly — frequent changes prevent signal detection. Mitigation: commit to the entire 8–12 week period.
- Assuming ‘limited’ equals contamination-free — factory shared lines are common. Mitigation: prefer brands stating “produced in dedicated lines.”
- Relying solely on blood/IgE tests — these are not diagnostic by themselves. Mitigation: Use an elimination diet as a diagnostic gold standard.
- Opening home-cooked diets without vet mistakes— risk of nutritional deficiencies. cure: consult a veterinarian or board-certified nutritionist, especially for young
- short to consider flavored blam or food, and often overlooked protein sources. Mitigation: ask your vet for a non-flavored option or check cargo carefully.
Safety warnings & accident signs
- Urgent veterinary attention if facial swelling, difficulty panting, collapse, or severe vomiting occurs — possible anaphylaxis.
- cubs & growth-stage dogs: do not initiate long-term home-cooked elimination diets without veterinary oversight due to growth needs.
- Rapid weight loss or poor demand during trial: contact your vet promptly; alternative action may be needed.
Breed & puppy debate
- Puppies require Dog-specific complete diets. Consult your vet before beginning restrictive or home-cooked remove diets.
- Breeds prone to skin disease: beagle, Terriers, Bulldogs, and Westies may need past referral to a veterinary dermatologist.
- Small or short, broad skull or muzzle breeds: palatability and feeding logistics can be challenging—use wet food or warmed kibble to improve acceptance.
Expert tips for European owners
- Prefer EU suppliers and products that explicitly declare compliance with regional nutritional guidance.
- Look for “single animal protein” labeling on packaging and avoid generic protein labels like “meat” or “poultry.”
- Check for shared equipment statements. Brands that produce in dedicated lines reduce cross-contact risk.
- Prescription hydrolyzed diets: buy through your clinic or verified distributors to avoid counterfeit or expired products.
- Cross-border shopping caution: check EU import rules and local regulations before importing pet food; customs and ingredient regulations vary by country.
FAQs
A: No universal “Best.” Start with a novel-protein limited ingredient diet for mild suspected cases. For confirmed or severe cases, vets often recommend hydrolyzed prescription diets.
A: Plan for 8–12 weeks for skin signs, with rechecks at 4 and 8 weeks. GI signs may improve sooner.
A: Generally, no, most allergies are protein-based. Grain-free diets do not reliably treat true food allergies and can bring other concerns.
A: Yes, if the product is truly single-protein and you can keep feeding strictly. For complex cases, prescription hydrolyzed diets are safer.
A: For mild cases, you can start an OTC novel-protein LID at home. For severe reactions, puppies, or hydrolyzed diets — see a vet.
A: Many flavored meds contain proteins. Ask your vet for non-flavored alternatives or ensure they match the trial protein.
Conclusion
If you suspect a food allergy right now — do this today:
- Start a symptom diary with daily photos and a one-line itch score.
- Remove all treats, chews, and flavored products from access.
- Choose a trial diet: OTC novel-protein LID for mild suspicion; discuss Hydrolyzed prescription with your vet for severe or complex cases.
- Commit to a strict 8–12 week trial and schedule rechecks at 4 and 8 weeks.
- If signs are clear, perform a supervised rechallenge to confirm the culprit.











